My first year as a mom has just come to an end. My husband, Jim, and I have been reminiscing for a few days about everything that happened this time a year ago. In honor of this monumental year, I wanted to share the story of how our beautiful boy, Owen, made his way into the world.
This isn’t the story I had told myself; the version where I would go into spontaneous labor at home one night in bed, tossing and turning through early contractions before telling Jim in the morning, “It’s happening!” We’d call the doula to our house later that day and stay home as long as possible, working gracefully through the contractions. I’d pet our dog, Moose, for comfort, and labor in our tub. We’d pull up to the hospital just before pushing, and stay for 36 hours tops.
Instead, at my 36 week appointment my blood pressure was slightly elevated, which had also happened around 28 weeks. Due to hospital policy and an abundance of caution, I was diagnosed with gestational hypertension, which is taken quite seriously because it can lead to preeclampsia. We scheduled two tests for the following day — a non-stress test, which would ensure Owen’s heart rate stayed steady over a 20-40 minute period of being monitored, and an amniotic fluid check, to ensure there was enough fluid around him to keep him safe. My assumption going into these tests was that if I “passed” we’d monitor my hypertension, (which I wasn’t convinced I had) and if I didn’t, we’d schedule induction. Turns out, induction was happening either way, and soon, it was just a question of being wheeled to Labor and Delivery right away, or coming back in a day or two.
It was New Year’s Eve when I got the call that my test results looked great, but that the midwives still wanted me to be induced. Tomorrow.
It hit me hard. I wasn’t yet prepared for delivery to be “any day now.” I had so much I wanted to do following the holidays. I was going to use my last 3 weeks of pregnancy to finish the nursery and wrap up some projects for my business. Instead, Owen was on his way, 3 weeks early. We asked if we could push to Monday (4 days from the call). The midwives allowed this, with the caveat that I would check my BP regularly, and that we’d come to the ER for induction if my readings took a turn.

We were told to come in for a BP reading where either number was over 150/90. My BPs were highest after we got the news of our induction, but tapered off over the next 2 days as I tried to reduce my stress.
We surrendered to this fate and began our final preparation. That last weekend without Owen feels like a lifetime ago. We washed and folded his clothes, rushed Amazon orders so we could pack our hospital bags, took long walks, and had big conversations about the life-changing event that was quickly approaching. There were fears and tears and after some processing, a good amount of excitement. We didn’t feel quite ready, but we quickly learned to drop every expectation we had been carrying with us, conscious or not, as new plans were underway.


MONDAY
During the day on Monday I did a couple “lasts,” including going out for hot chocolate and a pastry and blurting out — to a barista I had never met — “I’M HAVING A BABY TODAY!” Later, the extreme awareness of having my last dinner with my husband and parents before becoming a mom was surreal. I was so anxious. Like, clinically anxious: sweaty palms, tight chest, obsessive over-thinking. Zero chill.
Jim and I got to the hospital at 8pm and I was in my hospital bed by 9. We got cozy, because we knew what we were in for. First, this could take a while, and second, thanks to the pandemic, we would not be leaving our room (under any circumstance) until we were discharged. Plus, this was happening in January 2021, before most of the country was vaccinated. We had our masks on anytime anyone was in our room. I had to get covid tested the day before induction. No one could visit us in the hospital. Jim couldn’t go downstairs for a coffee. We would not breathe fresh air for days. And to our surprise, our first room in the antepartum unit (for pre-delivery care) was extremely compact, so my anticipatory anxiety around feeling cooped up was founded.


Induction is intentionally started late so that you can get a full night of rest while the drugs do their work, and ideally, you wake up the next day ready for some action. This wasn’t what happened for us. Little did I know, as I was panicking and unable to sleep that first night in anticipation of labor beginning, I’d sleep at the hospital for 3 nights before meeting Owen.
The first course of action was to take Misoprostol, which is a small dissolvable tab administered orally or vaginally that softens your cervix. Because I was being medically induced, my hopes of having a minimal intervention labor were out the window. I would be hooked up to monitors for the rest of my stay. The nice thing was that I could look over and see if I was having contractions. That night, I was woken up regularly by midwives and nurses giving me doses of Miso, doing cervical checks, and checking my blood pressure. I ended up getting a total of 3 hours of sleep in 1 hour increments.
TUESDAY
By morning, things were still uneventful. I had no dilation and only 30% effacement, which meant that my cervix was not opening and was also not softening. Around 9am, the team decided to take the next step by inserting a Foley balloon catheter. The catheter goes into the space above your cervix and below the baby, then inflates to 3 centimeters. It can stay there for up to 24 hours before needing to be removed, but for many people, it opens up the cervix much sooner, and falls out. Essentially, it forces dilation. To help things along, nurses will regularly tug on the Foley, and to create consistent tension when you move, the cord is taped to your inner thigh. Some women find the Foley installation, tugging, and tension to be extremely painful (along with the cervical progress checks) but I fortunately just found them to be entirely unpleasant.


Midday I was feeling pain synonymous with period cramping every 1-3 minutes and by 4pm I was breathing a little differently through each one. It was exciting that it felt like things were happening! At this point, we were transferred to L&D so we could begin Pitocin to move things further along. These interventions together generally jump start labor pretty effectively.
In the early evening, my Pitocin dosage was increased a few times and traction was applied to the foley. Cringe. I was feeling unpleasant contractions that made it hard to focus on anything but the pain. By 9:45, the midwife was paged for late decels, meaning that Owen’s heart rate was dipping with contractions (due to lack of oxygen) and could only return to baseline when I wasn’t contracting. He was not tolerating the Pitocin well. We reduced the level twice. Soon after, our nurse applied more pressure on my foley and it popped out. The 3cm bulb made its way through my cervix, which seemed promising. A lot of hip and back pain was relieved when the foley came out, and soon after, I lost my mucus plug.
Given all the recent developments, our midwife did another cervical check, but found there was no dilation. My foley did not work the way we thought it would. My cervix essentially shot it out and closed back up again. Great. And since the Pitocin was not tolerated, we were stuck somewhere between laughing at all the failed attempts, being impressed that my body was doing its job keeping Owen safe in my body to term, and also starting to feel demoralized.
After my foley fell out and my hip and back pain were relieved, I could no longer feel contractions. The foley seemed to have been putting just the right amount of pressure to make the contractions uncomfortable.
We had a long conversation late Tuesday night with our midwife about the lack of progress. She said she was unable to break my water to get things moving because the baby was too high. I was also deemed tachysystole, meaning my contractions were too close together when administering Pitocin. We could see them one after another on the monitor, and the lack of break was causing stress for Owen, leading to late and variable heart rate decelerations. We were told that Pitocin would be required to induce labor at this point, since the foley and Miso did not do enough on their own, and that if Owen couldn’t tolerate Pitocin the next day then we’d have to move to a cesarean delivery. I’ve since learned that 6mu of Pitocin is synonymous with spontaneous labor, and when we got up to a max of 5mu, we saw the late decels. I expressed fear of being pushed into a cesarean delivery, in a situation where I’m not even convinced I have hypertension and therefore no medical reason to be here doing this. The team decided to give Owen and my uterus a break for 3-5 hours, so Jim and I turned in for the night.
WEDNESDAY
After the 2am conversation with our midwife, and a shitty night of sleep in a crazy hospital bed that inflates and deflates in different places every 5 minutes (to neutralize your posture, I guess?!), we were up and administering a low dose of Pitocin just after 6am. The midwife on shift discussed the case with the new OB, who recommended we stop Pitocin and switch back to cervical ripening via Misoprostol. My cervix, at this point, was noted as “not favorable” in their notes. Grrrreat.
At 8am, I took the Miso dose. I decided to shower, have a big breakfast, change my clothes, and try to reset my mood. Despite my positive efforts, I was feeling emotional and overwhelmed with the induction process by late morning. I expressed feeling like we were going backwards and Jim and I decided to raise the question of being discharged. At this point, we’d taken every unnatural measure to force labor, and my body had clearly stated it wasn’t time. My request was to go home for one night. Breathe fresh air. Move my legs. Hug my dog. Sleep in my bed for a REAL night of sleep with no monitors and no middle of the night wakings and no possessed bed cushions. I felt like I was on the verge of a panic attack and that I needed to prioritize my mental health as I was soon to be thrown into the most important and consuming role of my life.
As we talked through it, I started to feel more calm. These were the moments that made me fall more in love with the midwife practice: we had countless hour-long conversations over our stay in the hospital, just for them to educate us and ease my anxiety. The way healthcare absolutely should be. I was reassured that a slow process is normal for a first time laboring person at 37 weeks but that our idea to go home was not unreasonable. The midwife discussed with the OB and while they felt my elevated BPs were mild, they ultimately decided they still wanted us to stay. If we left it would be against their medical advice.
We stayed, of course, and I did feel better after the shower and food. Another dose of Miso was administered while a cervical check was performed. I was at 1/30/-3 which means I was 1cm dilated, 30% effacement, and -3 fetal station. This essentially means no real sign of natural labor progressing.
Fetal station, that last measure, is used to indicate where the baby is in relation to the ischial spines in the pelvis. 0 station indicates the baby is level with the ischial spines and this is usually achieved when labor is beginning. When the baby is about to be delivered, they are at +5, meaning they’ve traveled 5cm below that starting point. Owen being positioned at -3 means he was 3cm above the ischial spines; too high. He had not “dropped,” as we say. Most babies drop naturally in the last couple weeks of pregnancy in preparation for delivery. I’m honestly impressed with how well my body tried to keep him safe and secure.

The nurse’s notes from 6pm state: “Patient is feeling less anxious. Has been working hard to do positive self talk. Spoke with her doula who was also reassuring. Smiling and engaged in conversation. Very supportive husband remains at bedside.” We were good. We were trying to have fun. We tried to treat what felt a bit like a jail cell more like an off-the-grid cabin in the woods. We were watching Soul, which had just come out, were trying not to check the news as the US Capitol was under attack (January 6, 2021), and we ordered Bar Cotto delivery for dinner. Another dose of Miso was administered around this time.
By the end of day 3, the themes of our stay were failed attempts at induction, Jim taking a lot of naps to rest up for our perpetually impending labor, Jim ordering “his hungry wife” a lot of “extra food” so he’d get free hospital meals (mine was free, he had to pay for his), Jim reading and playing chess on his phone, and me doing a lot of anxious waiting.
Suddenly, at 7pm, something made me laugh and my water broke. We went from not even being in early labor to it being time to push in a matter of 14 hours. The time scale is very blurry, but I remember my labor in a couple phases. Obviously, we had the waiting phase which has been extensively documented here. Once my water broke, we went into the “ooooohh, it’s happening! I’m excited!” phase. This turned into the “I need to vomit right now” phase. Then came the not super enjoyable “the pace of onset of pain has shocked my system and I am being traumatized by pain” phase, which quickly lead to all-out “BURN THE BOOKS GIVE ME THE EPIDURAL” phase. Then the peaceful final descent phase, thanks to modern medicine, and finally, the long and fairly volatile pushing phase.
The minute my water broke, there was a shift change for the nurses. (Note: this happened every 12 hours, so we’d met a lot of nurses and midwives by then!) Our new nurse essentially saw it go down and from then, things got pretty exciting. I remember feeling shocked, in a happy way, that something natural was happening. The measures we had taken to progress my labor certainly contributed to my water breaking, but my body had finally decided to surrender to the situation we found ourselves in.
I could swear I was puking into a plastic bag very shortly after this, but I do remember swaying in the rocking chair, bouncing on the ball, and trying different positions against the bed. I remember a good amount of alone time where I let Jim sleep and I took the onset of labor in stride, feeling each contraction wash over me.
By 9:30 I was having to pause and groan through my contractions. They were quickly becoming my primary focus. I was given another dose of Miso around 10:30 and my cervical check was unchanged: 1/30/-3. The nurse’s notes at 10:30 say I was squarely in early labor, and that I should spend the night resting, eating, and moving as tolerated.
THURSDAY
At 1:30am I texted my doula saying that I was unable to sleep through my contractions. I wasn’t yet huffing and puffing, but my contractions were 2-4min apart. In hindsight, I think I was going into active labor.
At 3am we called our doula to join us, finally, after days of her waiting to hear the word. By 3:30 the midwife’s notes said I had “difficulty coping,” so we did a cervical check to see where things were at. The results were essentially in line with someone who’s 38 weeks pregnant, not someone who’s going to push in a few hours: 1.5 cm dilated / 40% effacement / -2 station. I was shocked and discouraged — the pain was intensifying quickly, and I thought I had a high pain tolerance. How, I wondered, was early labor this painful?! We had a lengthy discussion between the all-consuming contractions about restarting Pitocin and when to consider pain management. I was scared to re-start Pitocin because of how much it would intensify my contractions and the possible impacts to Owen, but I agreed as they felt it was important to help move things along.
Pitocin started right away, and it very quickly did the job: sudden onset projectile vomiting (which is more commonly associated with later stage labor), back to back contractions with little break, and a complete inability to use any coping methods effectively. While the midwife notes at 5:30am state I was in “prolonged early labor” (I assume because of my confusing cervical check at 3:30) I believe I went through Pitocin-intensified, unmedicated transition in the bath (which was my last resort coping tool) without anyone knowing I was in later stage labor. They certainly knew I was in pain, given the exclamations, like “BURN THE FUCKING [unmedicated labor] BOOKS! WHO THE FUCK ARE THOSE [amazing, powerful] WOMEN! GIVE ME THE FUCKING EPIDURAL!”
Had I known that I was going to be fully dilated quite soon, I think I would have asked to cut the Pitocin and continue unmedicated, but I was being told I was so early in the process and I couldn’t imagine 10x-ing this pain. That felt impossible to bear.
My doula asked me a wise question at this point, the one thing I remember clearly outside of mentally burning books as a coping mechanism: “Is this pain causing you trauma? If it is, it’s time to talk about medicating.” My answer was a defeated — but certain — “yes.”
The epidural was a dream. I felt like a million bucks. The installation was a little creepy, and finding a quick moment to do it between contractions was logistically interesting. But my fears of feeling paralyzed didn’t come true. I wanted to be comfortable in bed after the night I just had. I rested for 2 hours under the premise that I was going to be in labor for another full day upon waking up. I also drank a lot of chicken broth, which I highly recommend. I had an unfounded anxiety about not being able to eat for days on end during labor, so this was a welcomed surprise.
Around 8, an absolutely stunning, glowing, golden sunrise came up over Capitol Hill, and I woke Jim up to let him know that Owen was almost ready. Our team was surprised to find that I was 9cm dilated and feeling rectal pressure with a growing desire to push. Surprisingly, Owen was still -1 station, so they positioned me to “labor down” for an hour to wait for him to lower.
By 9 I had reached completion — the whole 10cm. The energy grew in our delivery room with doctors, nurses, midwives, and students zipping in and out, Jim and our doula bedside, and me heading to an uncharacteristically zen place. I was excited. I felt so ready. My body knew exactly what to do. And I didn’t feel out of touch from the epidural like I feared; I could feel everything that happened, but the pain was manageable. I enjoyed the pushing stage because it was the final stretch. I was pushing out 9 months of ups and downs and physically forcing us into the next phase of our lives, a phase we had been ready for for quite some time. It was the end of a hard hospital stay, and the end of my pregnancy, and the start of our lives as a family of 3 (4 if you count the dog, like we do).
I was still on low dose Pitocin when first pushing, but Owen was again not tolerating it well. Because oxygen was restricted during his late decels and my contractions were back to back with no break, Owen essentially couldn’t breathe for an extended period of time. He wasn’t having time to recover before going into another contraction. The team placed a fetal scalp electrode monitor on his head so that they’d have a direct measure of his heart rate rather than using the unreliable monitor on my belly that had started to cause unnecessary anxiety in the room.
The Pitocin was stopped as a result, but soon after, my natural contractions became so far apart — 5-10 minutes! — that the progress I made while pushing seemed to almost reverse during the period before the next contraction. By 10am, Owen was only at 0 fetal station, so he had another 5cm to drop down.
The two non-ideal paths we could see forming ahead were (1) I wouldn’t progress enough with such spaced out contractions to get him out without surgery, or (2) we’d try to push him out more quickly with the help of Pitocin but he could become so intolerant of the intervention that we’d need to operate.
I credit our incredibly dedicated team for the measures they took to ensure a vaginal delivery. At 11, they restarted Pitocin after too many spaced out contractions with little progress. They encouraged a variety of positions to reduce the impacts to Owen, like leaning to one side, awkwardly bracing myself against the edge of the bed while pushing. We tried pushing every other contraction to give Owen a break. By 11:20, we had made it to +2 fetal station and by 12:30 he was +3 with 2cm of his head visible.

At this late stage, the team was worried he might be having cord compressions or perhaps the cord was around his neck, causing the “recurrent variables and late decels worsening with pushing over the last 15 minutes,” as our discharge notes stated. We discussed the vacuum in detail (which was extremely non-ideal for us), and we prepped me to be fully OR-ready. We turned Pitocin up and down as much as we could to walk the line between safety and finishing labor. At this point, my fear of the operating room was gone, but I was still laser focused on doing everything in my power to get Owen out right there on the bed. I felt strong the entire 4 hours I pushed. I found a lot of that strength surrounded by a room full of badass women delivering this baby. Every single person was doing their part.

Though I had chosen the midwifery practice for my pregnancy and delivery, I am eternally grateful that this particular on-call OB steered the ship. She took every measure possible. She was literally hands on, using perineal pressure to coach where I should be focusing my pushing. She walked me through everything that was going on in real time, and she trusted me when I said I could do exactly what she needed. When we were on the verge of the OR, we pulled back, we rested a moment, then we went really hard to make the progress that indicated to her we could finish safely. Those last few pushes were so much harder but so much more effective, and as Owen crowned, she reached in and pulled him out so we wouldn’t have to use the vacuum. I can still feel the feeling of him crowning and then suddenly disappearing from the birth canal. It almost felt like my body snapped right back to where it started. The physical absence of volume with him leaving my body shocked me.


I couldn’t believe we had made it, he was here, and I honestly didn’t know what to do. He had the sweetest cry and I can hear the exact sound of it to this moment. I was just saying “oh my god, oh my god” “look at him! oh my god!” and after a second I realized I could grab him, so I brought him to my chest. I was stunned and sobbing. Jim almost fainted he was so overcome with emotion. I didn’t know how to handle a minutes old baby. I couldn’t tell how fragile he was. So we just laid there.

Our firstborn, Owen James, was born at 12:54 on January 7th, 2021 to Neil Young playing in the background for the 13th time* after 4 hours of pushing. He was covered in vernix and looked just like his dad. He was and is the most beautiful baby I have ever seen.
*Don’t be like me and make your hospital playlist only 4.5 hours long.

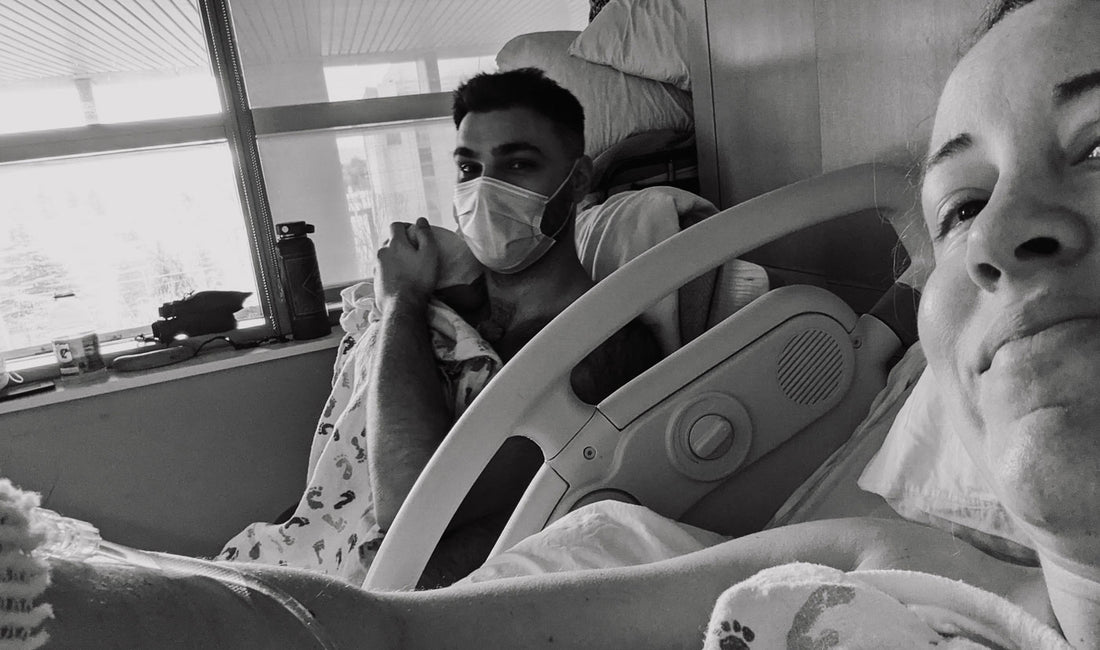
At some point during our initial period of bonding as a family of 3, I birthed my placenta without really noticing, and my second degree tear was stitched, right as my epidural was starting to wear off. Ouch. Owen was eventually in need of a little check-up, and I realized I was crashing very hard. I was exhausted and felt faint. I couldn’t imagine sleeping; no one wants to miss the biggest day of their life. I also couldn’t quite imagine eating or drinking because I was so past the point of hunger and exhaustion. The epidural started to wear off and I could walk around. We ordered a ton of food and I got some nourishment. Eventually we were wheeled to our postpartum room, and leaving the delivery room was by far the second best thrill of the day. Our 2 minute stroll to our new room felt like pure freedom. We stopped for a photo in front of the big Labor & Delivery sign with Owen, and settled into our 3rd room together, the one we thought we’d be in for a day before going home. That night, Owen got transferred to the NICU and we ended up staying several more days until he was well enough to go home. But that’s a story for a different day.


Our labor and delivery was a pretty wild ride. I feel very grateful that it was largely uncomplicated beyond being slow at the start, and a little bumpy at the end. It was the exact opposite of my plans, but I look back so fondly on the whole experience. I would relive January 7th again if I could. I’d visit that room and lay in that bed and eat that food and watch that movie and feel the before and after as deeply as I could.




3 comments
Awww Caylee, that was so beautifully written. I have tears streaming down my face, lying in bed, trying not o make sobbing sounds to wake Mark! Owen is a lucky boy, to be so loved by you and Jim. Thank you for sharing this; You have a perfect family, including Moose❤️
Loved reading your birth story as it wasn’t too different than mine. Refreshing and reminiscent. We are powerful women and it’s a nice reminder to know that we are not alone!
Just kicking off comments. I’d love to hear from others. Thanks so much for reading!